📞  — free, 24/7
— free, 24/7
 — free, 24/7
— free, 24/7
| Dosage | Package | Price per Dose | Price | |
|---|---|---|---|---|
| 500mg | 20 pills | A$48.08 | A$1,372.57 A$960.80 Best Price Popular | |
| 500mg | 10 pills | A$60.07 | A$859.39 A$601.58 |
This page provides general information about Xeloda. It is intended for patients and may need a prescription depending on local rules. Always follow your clinician’s instructions and check the official patient information leaflets supplied with your medicine.
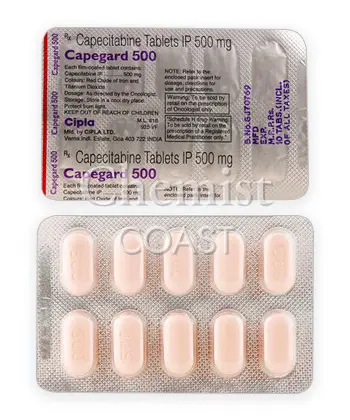
Xeloda is a brand name for the medicine capecitabine. It is a prescription chemotherapy medicine used to treat certain cancers. Your doctor will decide if Xeloda is appropriate for your treatment plan, based on your cancer type, stage, and overall health. Depending on local rules, access may require a prescription.
Capecitabine belongs to a class of medicines known as antimetabolites. It is taken by mouth as capsules. After you swallow the capsules, the drug is processed in the body and converted into an active substance that helps slow or stop cancer cell growth.
As with other chemotherapy medicines, Xeloda can affect not only cancer cells but also healthy cells. This is why it is important to take Xeloda exactly as prescribed and to discuss any side effects or concerns with your healthcare provider. If you have questions about how Xeloda fits with your overall cancer treatment, speak to your clinician or pharmacist.
Store Xeloda in its original packaging, at room temperature, away from moisture and heat. Keep the medicine out of reach of children. If you notice signs of damage to the tablets or packaging, contact your pharmacist before using it.
Xeloda may be prescribed for several cancer types where chemotherapy is appropriate. The exact use depends on the person’s cancer type, previous treatments, and the doctor’s plan. It may be used alone or in combination with other medicines as part of a treatment protocol.
In general terms, Xeloda is used in some cases of colorectal cancer and breast cancer, among other solid tumours. The decision to use Xeloda considers tumour characteristics, prior therapy, and the goal of treatment (for example, shrinking tumours, slowing progression, or palliating symptoms). Always rely on your clinician’s guidance for your specific situation.
The information given here is for general understanding and does not replace the official product information. If your doctor or pharmacist has given you different instructions, follow those exact directions. If you are unsure whether Xeloda applies to your cancer type, ask your treating team for a clear yes/no and the rationale behind the choice.
Keep your appointment schedule and blood tests as advised by your clinician. Ongoing evaluation helps determine how well the medicine is working and whether any dose adjustments or delays are needed. If you have questions about the aim of Xeloda in your therapy plan, discuss them with your doctor or pharmacist.
Xeloda is a prodrug. This means it is converted inside the body into an active chemical that interferes with the ability of cancer cells to make DNA, which is necessary for growth and division. The conversion is designed to happen more in cancer cells than in normal cells, to help limit some systemic effects.
The active form of Xeloda is a substance that helps to slow or stop cancer cell growth. Because the drug is active in cells that divide rapidly, it can also affect some normal cells that divide quickly. This can contribute to side effects, which your healthcare team will monitor and manage.
Tempo and pattern of drug activation depend on several factors, including how your body processes the medicine. Your clinician will consider these factors when planning treatment cycles. If you have questions about how Xeloda acts in your body, talk with your pharmacist or doctor.
Understanding how Xeloda works can help you recognise when side effects may occur and why certain monitoring tests are needed. Your healthcare team will provide specific information about what to expect during your treatment and when to seek help.
Take Xeloda exactly as prescribed by your clinician. The capsules are swallowed whole with a full glass of water. Do not crush or chew the capsules unless your healthcare professional has told you otherwise. If you have trouble swallowing, talk with your pharmacist about alternatives or strategies.
Medicines like Xeloda are usually given in cycles. A cycle may involve taking the capsules for a number of days, followed by a rest period. Your doctor will define the cycle length and the total number of cycles for your treatment. Do not alter the schedule unless advised by your clinician.
Take Xeloda with or after a meal, unless your doctor provides a different instruction. Consistency with meals helps with tolerability, but follow your prescribed timing. If you miss a dose, contact your clinician for guidance. Do not double the dose to make up for a forgotten one unless advised by a healthcare professional.
Store the capsules at room temperature and keep them in their original packaging. Keep them away from moisture and heat and out of reach of children. If the capsules are damaged or you notice a change in colour, contact your pharmacist before taking them.
If you have any side effects or symptoms that concern you while taking Xeloda, inform your clinician promptly. They may adjust your dose, spacing of cycles, or provide supportive care to manage side effects. Do not stop Xeloda on your own unless instructed by your healthcare team.
Xeloda may not be suitable for everyone. Your clinician will check for factors that could raise the risk of problems during treatment. This includes certain health conditions and current medications. If you have any concerns about suitability, discuss them with your doctor or pharmacist before starting therapy.
People with severe kidney or liver impairment may require special monitoring or dose adjustments. Your clinician will evaluate organ function through tests and clinical assessment to decide whether Xeloda is appropriate. Do not use Xeloda if you have a known allergy to capecitabine or any components of the medicine.
Pregnancy and breast feeding require careful consideration. In many cases, Xeloda may pose risks to a developing fetus or infant. If pregnancy is planned or suspected, inform your clinician promptly so that appropriate steps can be taken. Do not breastfeed while taking Xeloda unless advised otherwise by your clinician.
Other medicines you are taking can affect how Xeloda works or increase the chance of serious side effects. It is important to tell your doctor about all medicines, supplements, and herbal products you use. In some situations, Xeloda should not be used alongside specific therapies or may require adjustments.
If you have a history of severe reactions to chemotherapy, hand-foot syndrome, or other skin or nervous system problems, discuss these with your clinician. They can help determine whether Xeloda is suitable for you and outline monitoring plans during treatment.
Before starting Xeloda, tell your clinician about any medical conditions you have, including kidney or liver problems, heart disease, and recent surgeries. Your liver and kidney function tests may be performed to guide treatment decisions. If you notice new symptoms, report them promptly to your healthcare team.
Common dose-limiting side effects include rash on the hands and feet, mouth ulcers, and fatigue. In some people, these effects can be more serious and require dose adjustments, temporary stopping, or additional care. Your clinician will monitor for these possibilities and manage them accordingly.
Dehydration, electrolyte imbalances, and diarrhea can occur with Xeloda. It is important to maintain fluids and contact your clinician if you develop persistent or severe symptoms. Infections, fever, or signs of a reduced immune response should be reported promptly, as treatment may be paused or adjusted.
Because Xeloda is processed through the body in a way that targets rapidly dividing cells, blood counts may fall. Your doctor will monitor blood tests and may adjust the treatment plan to reduce risks such as infections or bleeding. Follow up appointments and tests are an essential part of the treatment plan.
Tell your clinician about all medicines you are taking, including over-the-counter drugs, vitamins, and herbal products. Some medicines can interact with Xeloda, increasing side effects or reducing effectiveness. Do not start new medicines without discussing them with your healthcare team.
Like other chemotherapy medicines, Xeloda can cause a range of side effects. Some people experience only mild effects, while others may have more noticeable changes. Your clinician can help manage side effects to keep you as comfortable as possible during treatment.
Common side effects include tiredness, loss of appetite, nausea, vomiting, diarrhea, and stomach discomfort. You may notice changes in your hair, nails, or skin. Mouth sores or a sore throat can occur, and you might have a flattened sense of taste. These effects are usually temporary but should be reported if persistent or worsening.
Other frequently reported effects are hand-foot syndrome (redness, swelling, and pain on the palms of the hands or soles of the feet), rash, and infections due to lower white blood cell counts. Your clinician may suggest supportive care measures to help with these problems and may adjust your treatment if needed.
Less common side effects include changes in liver enzymes, elevated blood sugar, dehydration, dizziness, and changes in mood or sleep. If you notice yellowing of the skin or eyes, severe abdominal pain, or any signs of severe infection, seek urgent medical help or contact your clinician immediately.
Serious reactions requiring urgent medical attention can occur in rare cases. Call your clinician right away if you experience chest pain, severe shortness of breath, severe diarrhea with dehydration, signs of an allergic reaction (such as swelling of the face or throat, severe rash, or trouble breathing), or any new, severe symptoms. These events require prompt assessment and may necessitate stopping treatment or adjusting the plan.
Tell your clinician about all medicines you take, including prescription drugs, over-the-counter medicines, vitamins, and herbal products. Some medicines can interact with Xeloda and alter how it works or increase the risk of side effects. Your clinician can review these interactions and adjust your plan if needed.
Medicines that affect blood clotting, such as warfarin, may interact with Xeloda and change bleeding risk. Your doctor will monitor your blood tests and may adjust doses or timing of treatments if you are taking anticoagulants.
Concomitant chemotherapy, radiation therapy, or other cancer medicines can influence how Xeloda works. In some cases, combining therapies improves outcomes; in others, it increases toxicity. Always follow your clinician’s guidance about combining treatments and reporting any new medicines you start during Xeloda therapy.
Some drugs can affect the way capecitabine is processed in the body or increase the chance of side effects. This includes certain enzymes in the liver and other medicines that raise the risk of dehydration or kidney strain. If you are unsure whether a medicine you plan to take is safe with Xeloda, ask your pharmacist or clinician before use.
Do not start new supplements or herbal products without discussing them with your clinician, as some can interact with chemotherapy. If you experience symptoms that you think may be related to an interaction, contact your healthcare team for advice.
Pregnancy may present a serious risk to the developing fetus if Xeloda is used. If you are pregnant, planning a pregnancy, or are breastfeeding, discuss these plans with your clinician before starting treatment. In many cases, effective contraception is advised during Xeloda therapy and for a period after completion, as advised by your doctor.
Breastfeeding while taking Xeloda is generally not recommended, as the medicine may pass into breast milk and affect a nursing infant. If you are breastfeeding or plan to breastfeed, speak with your clinician about the risks and alternatives.
If you become pregnant while taking Xeloda, contact your clinician immediately to discuss the next steps. They will help determine if there is a need to continue treatment or to pause therapy during pregnancy.
For people who can become pregnant, it is important to use effective contraception during treatment and for a period after finishing therapy, as advised by your clinician. If you have questions about fertility and Xeloda, discuss them with your doctor before starting treatment or during the course of therapy.
Responses to cancer medicines vary between individuals. Some patients see changes over weeks, while others may take longer. Your clinician will monitor your response through examinations and tests and discuss results with you.
If you miss a dose, contact your clinician for specific guidance. Do not double the dose to compensate for a missed one unless advised by a healthcare professional. Maintaining the planned schedule helps balance effectiveness and side effects.
In many treatment plans, Xeloda is used in combination with other medicines. Your clinician will design a plan that considers potential interactions and the goals of therapy. Do not start or stop other medicines without consulting your healthcare team.
Specific dietary restrictions are not universally required with Xeloda. Some people find that meals help with tolerability. Your clinician may offer advice on hydration, nutrition, and managing side effects during treatment.
Hand-foot syndrome presents as redness, swelling, or pain on the palms or soles. If you notice these symptoms, contact your clinician promptly. Your treatment plan may be adjusted to reduce discomfort and prevent progression.
Cycles vary by treatment plan and cancer type. Your clinician will outline the cycle length and the total number of cycles. It is important to attend follow-up visits and tests so that the plan can be tailored to your response and tolerance.
Severe diarrhea or dehydration requires medical attention. Contact your clinician or seek urgent help if you cannot keep fluids down, have signs of dehydration, or if stools are very frequent or bloody. They may adjust treatment or provide supportive care.
Travel is usually possible, but plan ahead. Bring enough medication for the trip, keep it in its original packaging, and carry any necessary medical documents. If you have to change time zones or meals, notify your clinician so they can advise on managing the regimen safely.
Routine blood tests are commonly advised during chemotherapy to monitor blood counts and organ function. Your clinician will schedule these tests and discuss results with you, including any required adjustments to the treatment plan.
New or worsening symptoms should be discussed with your clinician. This includes fever, persistent vomiting, severe abdominal pain, pale skin, or unusual bleeding. Early reporting helps manage side effects and protect your overall health.
Information on Xeloda is based on general product information and commonly used clinical practice guidelines. If you require official and detailed references, consult your prescriber and the patient information leaflet provided with the medicine.
Australian Medicines Handbook and national regulatory patient information are commonly used resources to inform healthcare professionals and patients about capecitabine therapy. Your treating team can guide you to the most relevant, up-to-date sources for your situation.
Always rely on your doctor, pharmacist, or the official product documentation for safety, dosing, and monitoring details specific to you. If you have questions about how Xeloda applies to your case, speak with your clinician for personalised information.
14–21 days. Free from A$279.23 .
5–9 days. A$41.88
−10% when paying with cryptocurrency.
−10% on all repeat orders.
All orders are packed in neutral, unbranded boxes with no product name on the outside.
